The American Registry: 2022 America’s Most Honored Doctors – The Best of the Best Award Seen Here Honoring Our Doctors.
Psychiatry News & Updates
Dr. Dholakia, MD: Castle Connolly Top Doctor 2022
Dr. Dholakia, MD: Castle Connolly Top Doctor 2022 is honoring our top doctors here at Orange Psych Associates.
The U.S. Surgeon General’s Framework for Workplace Mental Health & Well-Being 2022
The U.S. Surgeon General’s Framework for Workplace Mental Health & Well-Being 2022
Your Child’s Medication: How to Help Organize and Manage Their Treatment
Your Child’s Medication: How to Help Organize and Manage Their Treatment
Orlando’s Elite Doctors 2022
Orlando’s Elite Doctors 2022 recognize Our Doctors
AACAP Statement on SCOTUS Decision Overturning Roe v. Wade
Washington, DC, June 24, 2022 – The American Academy of Child and Adolescent Psychiatry (AACAP) is disappointed, saddened, and outraged by today’s...
Congress Must Address Two National Crises: Gun Safety and Mental Health
Congress Must Address Two National Crises: Gun Safety and Mental Health %%sitename%%
Pediatricians, Child and Adolescent Psychiatrists and Children’s Hospitals Declare National Emergency in Children’s Mental Health
Pediatricians, Child and Adolescent Psychiatrists and Children’s Hospitals Declare National Emergency in Children’s Mental Health
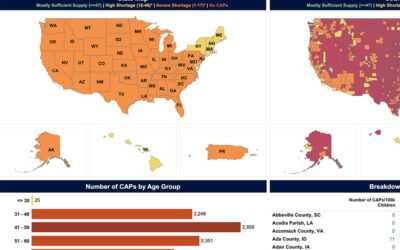
Severe Shortage of Child and Adolescent Psychiatrists Illustrated in AACAP Workforce Maps
Severe Shortage of Child and Adolescent Psychiatrists Illustrated in AACAP Workforce Maps